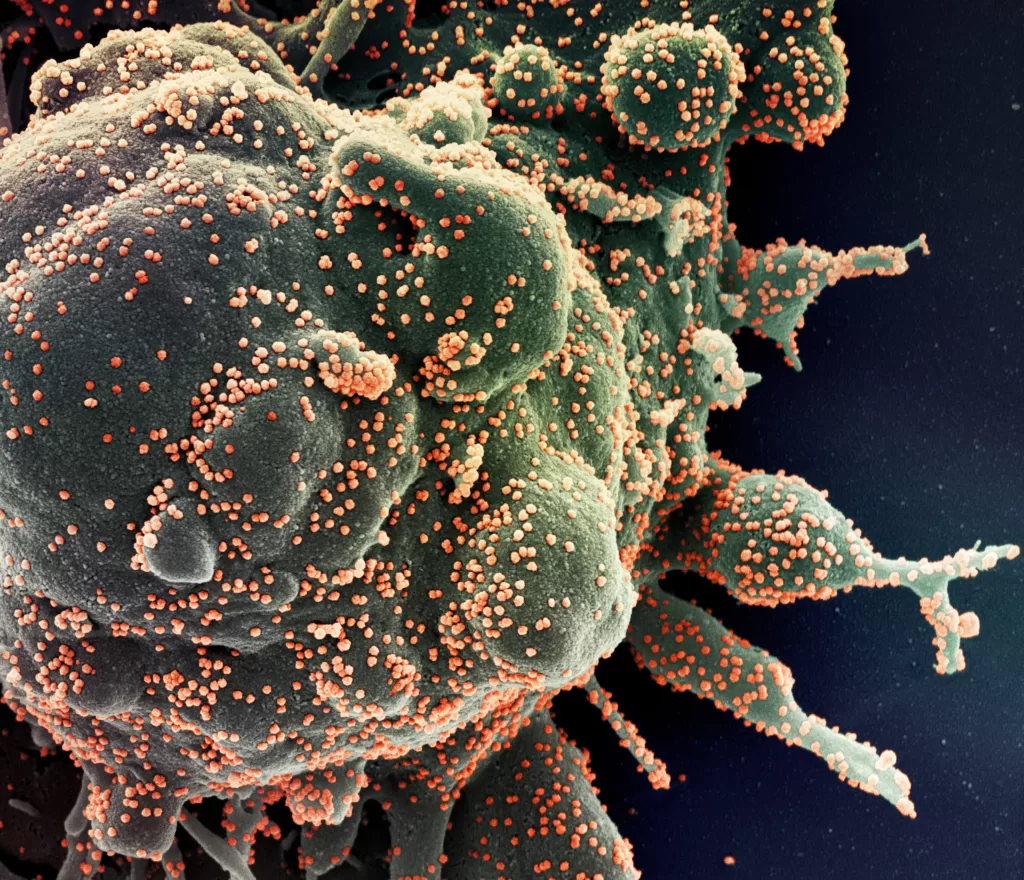
Why India has most to gain from beating antimicrobial resistance
India is the 'world capital' of antimicrobial resistance and now part of a global fight to save millions of lives and trillions of dollars.
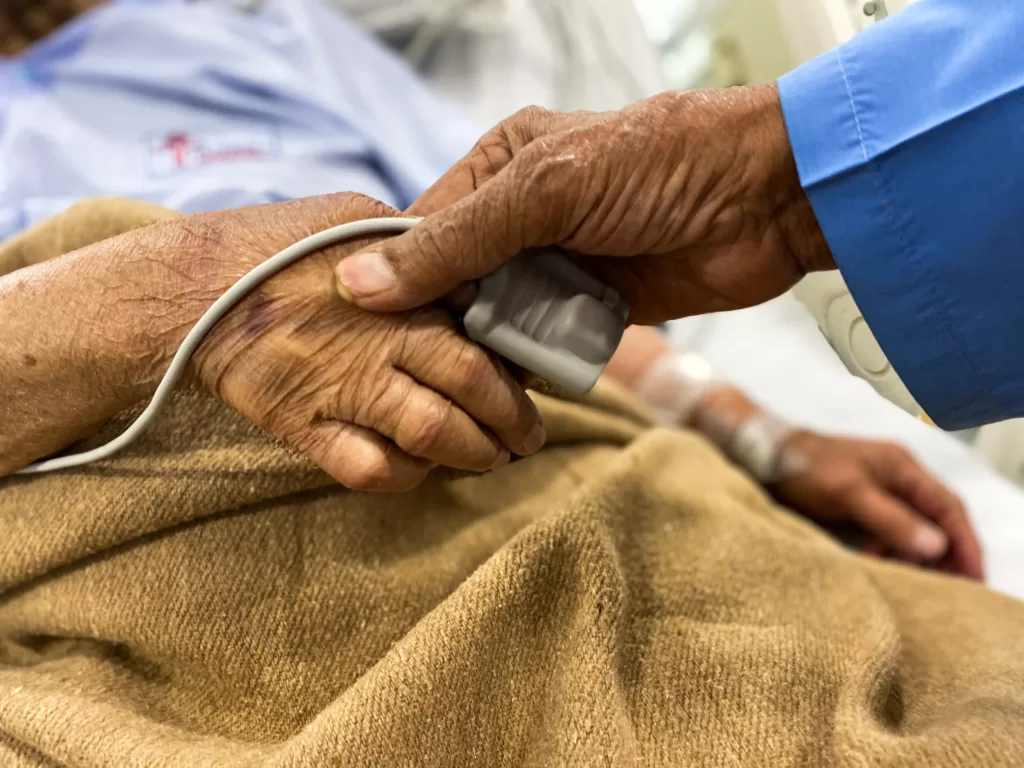 Enhancing access to quality healthcare is one way India can fight back against antimicrobial resistance. : Pexels: Muskan Anand https://www.pexels.com/license/
Enhancing access to quality healthcare is one way India can fight back against antimicrobial resistance. : Pexels: Muskan Anand https://www.pexels.com/license/
India is the ‘world capital’ of antimicrobial resistance and now part of a global fight to save millions of lives and trillions of dollars.
Antimicrobial resistance stands as one of the most pressing global health concerns. However, it is in developing and economically challenged nations that the true impact of this issue is felt most deeply.
Antimicrobial resistance is a health problem potentially worse than the recent COVID-19 pandemic. India bears the unfortunate distinction of hosting a significant burden of antimicrobial resistance.
However, the nation has earnestly embraced the challenge of addressing AMR, recognising the urgent need for attention to this issue.
Antimicrobial resistance refers to the ability of microorganisms like bacteria, viruses, fungi and parasites to become drug resistant, or so-called ‘superbugs’.
If drugs cannot treat microbial infections, then deaths from tuberculosis, malaria, cholera and other diseases will skyrocket. Already there are seven million annual deaths globally due to bacterial infections.
Antimicrobial resistance is part of a natural evolutionary process as microbes find ways to outsmart the drugs intended to combat them. Microbes are microscopic living organisms that are invisible to the naked eye yet have co-evolved with humans and play vital roles in maintaining life on Earth.
Many microbes are essential for human existence, but specific types can cause infectious diseases, leading to millions of deaths.
As scientific comprehension of microbial entities has progressed, so have the approaches to tackling them through new treatments.
In their ongoing struggle for survival, microbes have in turn evolved mechanisms to become drug resistant.
Over the past century, antibiotics have achieved remarkable milestones in the medical realm, revolutionising global healthcare. That journey started in 1928 with Alexander Fleming’s discovery of penicillin, leading to clinical application by the 1940s and earning him a Nobel Prize with Howard Florey and Ernst Chain.
Subsequent discoveries included antibiotics like streptomycin (1944), tetracycline (1948), and erythromycin (1952), bolstering our arsenal against infections.
However, fewer new types of antibiotics emerged in later decades, and the approval of new antibiotics further decreased going into the 21st century. Only two — telavancin and ceftaroline fosamil — were introduced.
The search for new antibiotics has been hindered by the intricate science involved, hefty development costs and reduced incentives. In this environment, antimicrobial resistance has emerged as a formidable threat, complicating the development of new drugs.
The World Health Organization estimates antimicrobial resistance could already be responsible for 700,000 deaths a year. An alarming 400,000 of these fatalities could be in developing nations.
If unaddressed, by 2050 antimicrobial resistance might claim around 10 million lives, with 80 percent of cases likely to be in developing regions.
In comparison, the COVID-19 pandemic has led to around seven million reported deaths in about three years.
Antimicrobial resistance also poses a huge economic threat, potentially causing global GDP to drop by between 2 and 3.5 percent and the livestock industry by 3 to 8 percent.
That’s a cumulative USD$100 trillion loss by 2050. Clearly, global action is needed against antimicrobial resistance to safeguard lives and protect the economy.
India is seen virtually as the home of antimicrobial resistance.
Along with many low-income and developing nations, it is also grappling with drug-resistant tuberculosis, malaria and cholera, exacerbated further by poverty, illiteracy, overcrowding and malnutrition.
Limited awareness and restricted healthcare access have led to antimicrobial self-medication in India, which is fuelled by unregulated access to over-the-counter drugs. Even in the health system patients often receive broad-spectrum antimicrobials due to insufficient diagnostics.
Low doctor-to-patient ratios and the absence of infection prevention and control guidelines contribute to increased transmission of drug-resistant strains.
All of this has compounded the antimicrobial resistance crisis.
The excessive use of antibiotics in poultry, livestock and agriculture adds another dimension to the problem and means ensuring judicious antibiotic usage in these sectors crucial to protecting both human and animal health.
Despite the gravity of the antimicrobial resistance threat and scientific advances, the development of new classes of antibiotics has been slow.
The pharmaceutical industry is generally reluctant to invest in antibiotic research and development because it involves more than a decade of meticulous research and clinical trials and can cost more than a billion dollars.
And the return on that investment is often seen as relatively limited, especially compared with drugs used for chronic conditions like cancer and diabetes that promise extended usage and greater revenue.
There are 77 new molecules in clinical trials and only 32 of these are non-traditional antibiotics. That compares with more than 10,000 molecules in clinical trials for cancer, more than 1,800 for neuropsychiatric conditions, and over 1,500 for blood immune disorders.
Antimicrobial resistance is itself another major challenge because it rapidly diminishes the effectiveness of new antibiotics and makes it hard to recoup development costs.
Stringent regulatory requirements for antibiotic approval also extend the development process and add to costs.
Despite the economic challenges for the pharmaceutical industry, new strategies to tackle antimicrobial resistance still have to be found.
All stakeholders, including pharmaceutical companies, must collaborate to discover new antibiotics for the greater good.
The World Health Organization estimates about 3.5 million individuals in developing nations suffered from infections caused by drug-resistant bacteria in 2016.
Developed countries, including select European nations and the United States, contend with notably fewer instances, owing to superior health infrastructure, rigorous infection control measures and more regulated antibiotic usage.
In 2018, India took a strategic step to combat antimicrobial resistance.
The Ministry of Health issued regulations for responsible dispensing of antimicrobials. These measures need stringent enforcement.
India had introduced the National Action Plan on Antimicrobial Resistance in 2017, aiming to raise awareness, enhance infection control measures and encourage rational antibiotic use.
The issue also has a significant place on the G20 health agenda during India’s presidency. Over the past decade, governments worldwide have made efforts to seriously address the challenge.
The antimicrobial resistance challenge required a multifaceted approach in developing countries like India.
Strengthening healthcare infrastructure and enhancing access to quality healthcare, advocating responsible antibiotic use, boosting infection prevention and control measures, and investing in surveillance systems are pivotal strategies.
Thinking globally, a coordinated effort that involves governments, healthcare professionals, pharmaceutical firms and international organisations is imperative.
Antimicrobial resistance could very well be the next pandemic that humanity faces.
V S Chauhan is President of the Malaria Vaccines Development Program. He is also the Chancellor of GITAM University, Co-Founder of Biotide Solutions LLP and a Distinguished Visiting Professor at the Institution of Eminence University of Delhi.
Originally published under Creative Commons by 360info™.